Cervical Spondylosis
Cervical spondylosis is age-related wear on the cartilage, discs, and bones of the neck. By age 60, most people show some radiographic evidence of it, though many never develop symptoms. As discs lose water content and height, vertebrae can develop bone spurs that crowd the spinal canal or the openings where nerve roots exit. When these changes cause symptoms—neck pain, arm numbness, weakness—the condition is sometimes called cervical osteoarthritis or degenerative disc disease of the neck.
Find a Specialist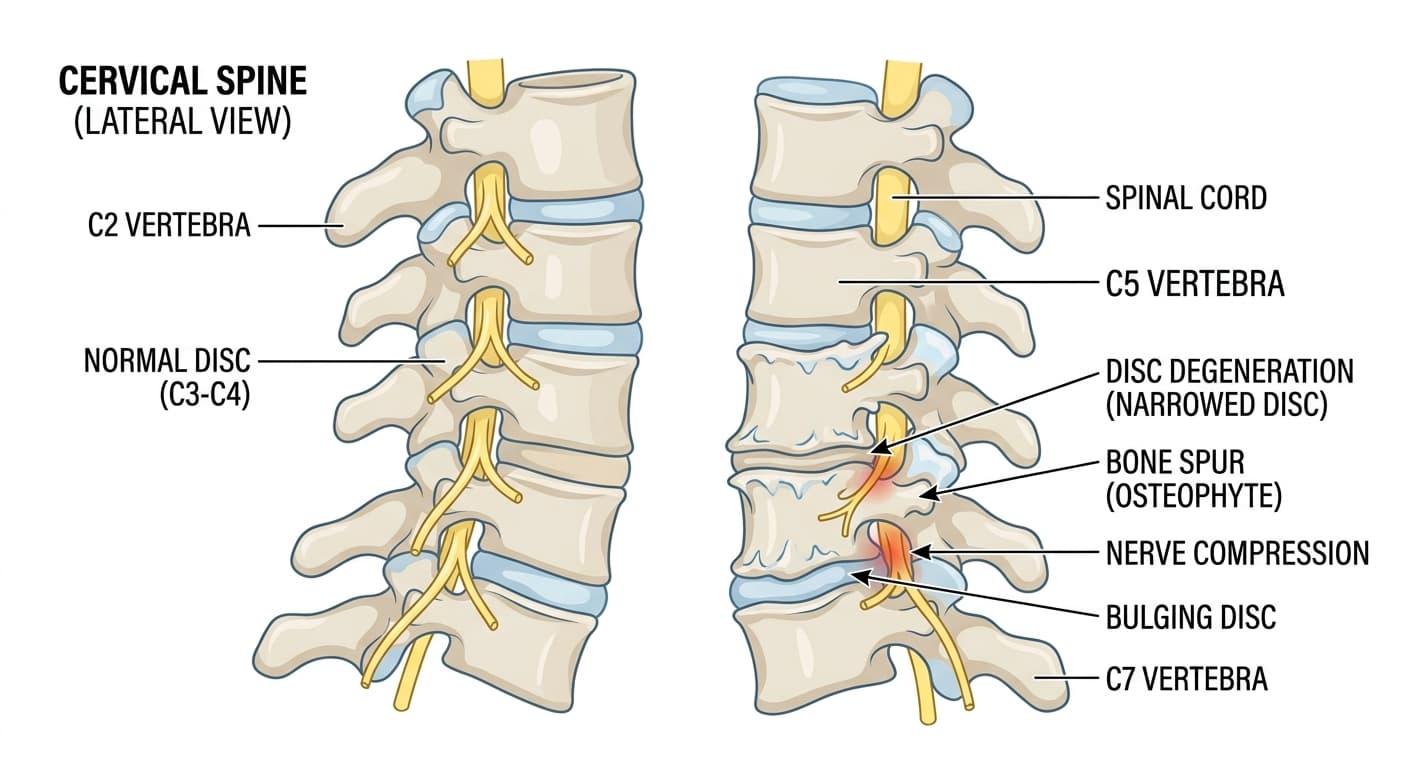
Symptoms
- Neck stiffness and pain, often worse in the morning
- Aching or grinding sensation with neck movement
- Headaches starting at the base of the skull
- Numbness, tingling, or weakness in one or both arms or hands
- Loss of grip strength or difficulty with fine motor tasks
- In severe cases, problems with balance or walking (cervical myelopathy)
When to See a Doctor
See a spine specialist if neck pain is persistent and limiting your daily activities, if you have arm or hand symptoms suggestive of nerve compression, or if you notice any changes in your balance, coordination, or bladder or bowel function—the last of these warrants urgent evaluation.
Treatment Options
Physical therapy
Targeted exercises to strengthen neck and shoulder muscles, improve posture, and decompress the cervical spine. Mainstay of initial treatment for most patients.
Medications
NSAIDs for pain and inflammation, muscle relaxants for spasm, and occasionally short courses of oral steroids for acute nerve flares.
Cervical epidural steroid injection
Steroid injected near the affected nerve root to reduce inflammation and provide weeks to months of relief. Often used when oral medications fail or when more precise targeting of a specific level is needed.
Surgery
Considered when conservative treatment fails after several months, or when there is progressive neurological deterioration. Options include anterior cervical discectomy and fusion (ACDF) or cervical disc replacement, depending on the number of levels involved and patient anatomy.
Recovery Timeline
Most patients with mild to moderate symptoms respond well to conservative treatment within 6–12 weeks. Surgical recovery varies: ACDF patients are typically released the same or next day, with a return to desk work in 2–4 weeks and full activity in 3–6 months. Cervical disc replacement has a similar timeline.
Frequently Asked Questions
Is cervical spondylosis the same as a herniated disc in the neck?
Not exactly. A herniated disc is one specific finding that can occur as part of cervical spondylosis, but spondylosis also includes bone spurs, disc height loss, and facet joint arthritis. A herniated disc can happen in a young person from a single injury; spondylosis is cumulative wear that develops over decades.
Does cervical spondylosis always get worse?
Not necessarily. Many people have significant radiographic spondylosis with no or minimal symptoms that stay stable for years. Symptoms can fluctuate—improving with physical therapy and activity modification—and do not always progress linearly. The correlation between imaging findings and symptoms is imperfect; a dramatic MRI does not guarantee dramatic symptoms.
What type of doctor treats cervical spondylosis?
Spine surgeons (either orthopaedic or neurosurgical), physiatrists, and neurologists all manage cervical spondylosis. Start with a spine specialist if you have significant arm symptoms or any concern about spinal cord involvement. Primary care can manage mild, stable neck pain initially.
Related Specialty
Spine Specialists →Related Procedures
Cervical Spondylosis by State
Related Conditions
This information is for educational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.