Spondylolisthesis
Spondylolisthesis is a condition where one vertebra slips forward over the vertebra below it. The slip disrupts the normal alignment of the spine and can compress nerves exiting the spinal canal. Severity ranges from a minimal slip (Grade I, less than 25%) to complete displacement (Grade V). The most common types are isthmic spondylolisthesis—from a stress fracture in young athletes—and degenerative spondylolisthesis—from worn facet joints in adults over 50.
Find a Specialist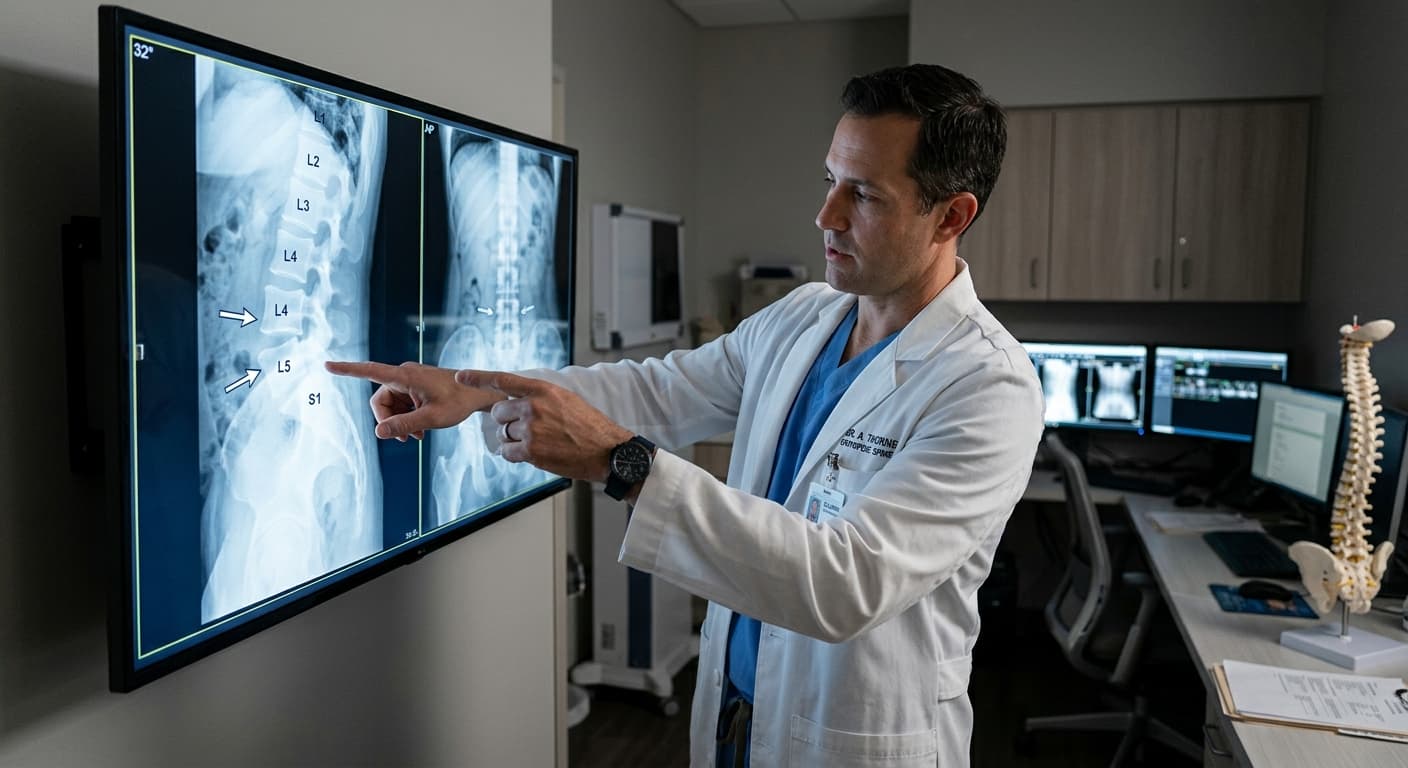
Symptoms
- Low back pain that worsens with standing and walking, improves with sitting
- Pain, numbness, or tingling radiating into the buttocks or legs (if nerves are compressed)
- Muscle tightness in the hamstrings
- In advanced cases, a visible step-off or forward shift in the lower back
- Difficulty walking for long distances
- Leg weakness in severe cases
When to See a Doctor
See a spine specialist if low back pain is accompanied by leg pain, numbness, or weakness—these suggest nerve compression from the slipped vertebra. If you have been told you have spondylolisthesis and develop bowel or bladder changes, go to an emergency room immediately as this indicates cauda equina syndrome.
Treatment Options
Physical therapy
Core strengthening, hamstring flexibility, and lumbar stabilization exercises reduce stress on the slipped vertebra and often control symptoms effectively for Grade I and II slips.
Pain management and injections
NSAIDs, activity modification, and epidural steroid injections can provide significant relief from nerve-related symptoms while pursuing conservative care.
Spinal fusion surgery
Indicated for Grade III–IV slips, progressive neurological symptoms, or failure of 6+ months of conservative treatment. The slipped vertebra is stabilized with rods and screws, and a bone graft fuses the two vertebrae together. Minimally invasive approaches are used when possible.
Recovery Timeline
Conservative treatment often provides good control of symptoms over weeks to months. Spinal fusion recovery: hospital stay 2–4 days, return to light activity in 4–6 weeks, full recovery and fusion completion in 3–6 months. Return to heavy work or sport is typically 6–12 months post-surgery.
Frequently Asked Questions
What is the difference between spondylolisthesis and spondylolysis?
Spondylolysis is a stress fracture in the bony arch of the vertebra (the pars interarticularis) without any forward slip. Spondylolisthesis occurs when that stress fracture—or disc and joint degeneration—allows the vertebra to actually slide forward. A person can have spondylolysis that never progresses to spondylolisthesis, or the fracture can allow slippage over time.
Can spondylolisthesis get worse over time?
It depends on the grade and type. Most adult degenerative spondylolisthesis is stable and does not progress significantly. Isthmic spondylolisthesis in younger patients has a higher risk of progression, particularly during the adolescent growth spurt. High-grade slips (Grade III+) are monitored more carefully and have a greater chance of requiring surgery.
What type of doctor treats spondylolisthesis?
Orthopaedic spine surgeons and neurosurgeons treat spondylolisthesis. Physiatrists (physical medicine and rehabilitation physicians) and spine-specialized physical therapists manage conservative care. For most patients with mild to moderate symptoms, non-surgical treatment with these providers is the right first step.
Related Specialty
Spine Specialists →Related Procedures
Spondylolisthesis by State
Related Conditions
This information is for educational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.