Dupuytren's Fasciectomy
Dupuytren's fasciectomy removes the thickened fibrous tissue (diseased fascia) in the palm that pulls the fingers into a bent position. In Dupuytren's contracture, cords of abnormal collagen form under the skin of the palm, progressively drawing the ring and small fingers toward the palm. Fasciectomy is the most established surgical treatment: the surgeon excises the diseased cords through an incision in the palm, releasing the finger contracture. Needling (percutaneous aponeurotomy) and collagenase injection (Xiaflex) are less invasive alternatives but have higher recurrence rates.
Find a Surgeon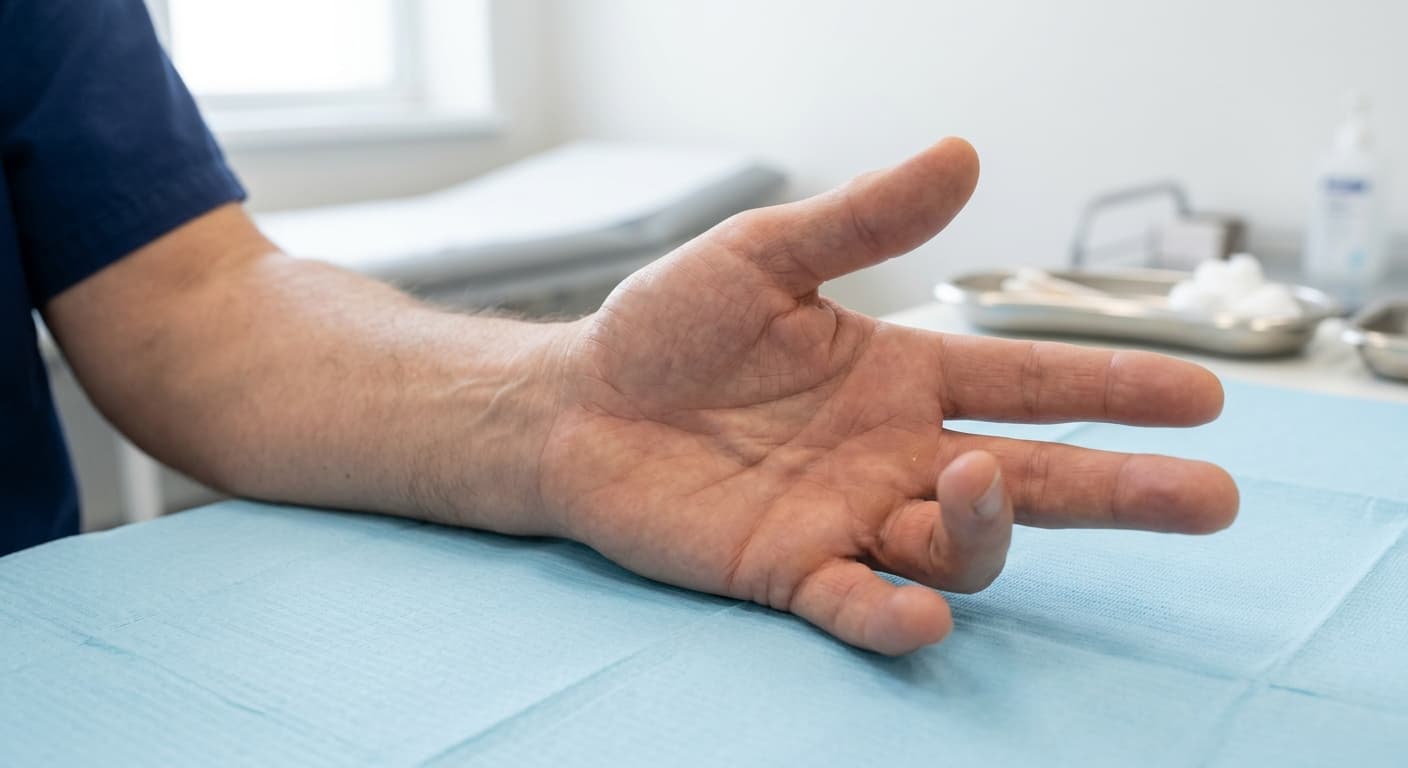
Who Needs Dupuytren's Fasciectomy?
Patients with Dupuytren's contracture causing a contracture of 30 degrees or more at the metacarpophalangeal (MCP) joint, or any contracture at the proximal interphalangeal (PIP) joint. The "tabletop test" is a practical benchmark: if you cannot lay your hand flat on a table, the contracture is functionally significant. Surgery is typically deferred until the contracture limits daily activities — grip, handshakes, or inserting the hand into a pocket.
What to Expect
Recovery Timeline
Hand elevation to control swelling. Fingers are splinted in extension. Some patients report significant post-operative swelling and discomfort.
Wound check. Sutures removed or dissolving. Hand therapy starts: scar massage, gentle range-of-motion, custom splint fabricated.
Progressive extension exercises. Night splinting continues for 3-6 months to prevent recurrence. Grip strength gradually returns.
Return to light work. Incision remodeling continues. Scar sensitivity (sensitivity to touch and cold) is common and usually resolves over months.
Return to full hand function for most patients. Stiffness in the PIP joint can be slower to resolve — particularly if the PIP had a significant pre-operative contracture.
Risks & Complications
- Wound healing problems — Dupuytren's skin is thin and adherent, making closure more complex
- Nerve injury causing numbness or tingling in the finger
- Artery injury (digital arteries run close to the diseased cords)
- Complex regional pain syndrome (CRPS) — a disproportionate pain response
- Recurrence — Dupuytren's has a biological recurrence rate of 40-70% at 5-10 years regardless of technique
- Stiffness in the PIP joint that does not fully correct even after the cord is released
Frequently Asked Questions
Will Dupuytren's contracture come back after surgery?
Dupuytren's is a genetic condition affecting the way your body produces collagen; surgery removes the disease from a specific area but doesn't change the underlying biology. Recurrence at the operated site or new involvement in other fingers is common — roughly 40-70% of patients see some recurrence within 5-10 years. The less invasive procedures (needling, collagenase injection) recur faster and more completely than fasciectomy. Patients with earlier onset, bilateral disease, and ectopic disease (knuckle pads, Ledderhose in the foot) tend to have more aggressive disease.
What is the difference between fasciectomy, needling, and Xiaflex?
Needling (percutaneous aponeurotomy) uses a needle to break the cord percutaneously — it is office-based, has minimal recovery, but the cord is not removed so it recurs more quickly. Xiaflex (collagenase injection) injects an enzyme that dissolves the cord; the finger is then manipulated straight. It is FDA-approved for MCP joint contractures and some PIP contractures. Fasciectomy removes the cord entirely and generally achieves better correction of PIP contractures, but recovery is longer. For most patients with functional MCP contractures, needling or Xiaflex is offered first; fasciectomy is typically reserved for severe or recurrent cases.
How long does hand therapy last after Dupuytren's surgery?
Most patients attend formal hand therapy for 6-12 weeks and continue home exercises and night splinting for 3-6 months. The splinting is important — without it, the finger tends to drift back toward flexion as the wound scars down. Compliance with the night splint is one of the strongest predictors of maintained correction at 1 year.
Find a surgeon for Dupuytren's Fasciectomy
Compare orthopaedic surgeons who perform this procedure.
Search surgeonsEstimated Cost
$8,000 - $20,000. Covered by most insurance when functional deficit is documented. Single-digit fasciectomy is less expensive than multi-digit procedures. Collagenase injection (Xiaflex) is an insurance-covered alternative for some single-cord contractures at the MCP joint.
Full cost breakdownRelated Specialty
Hand Specialists →Related Conditions
Other Procedures
This information is for educational purposes only. Costs are estimates and vary by location, surgeon, and insurance. Always consult a qualified healthcare provider.