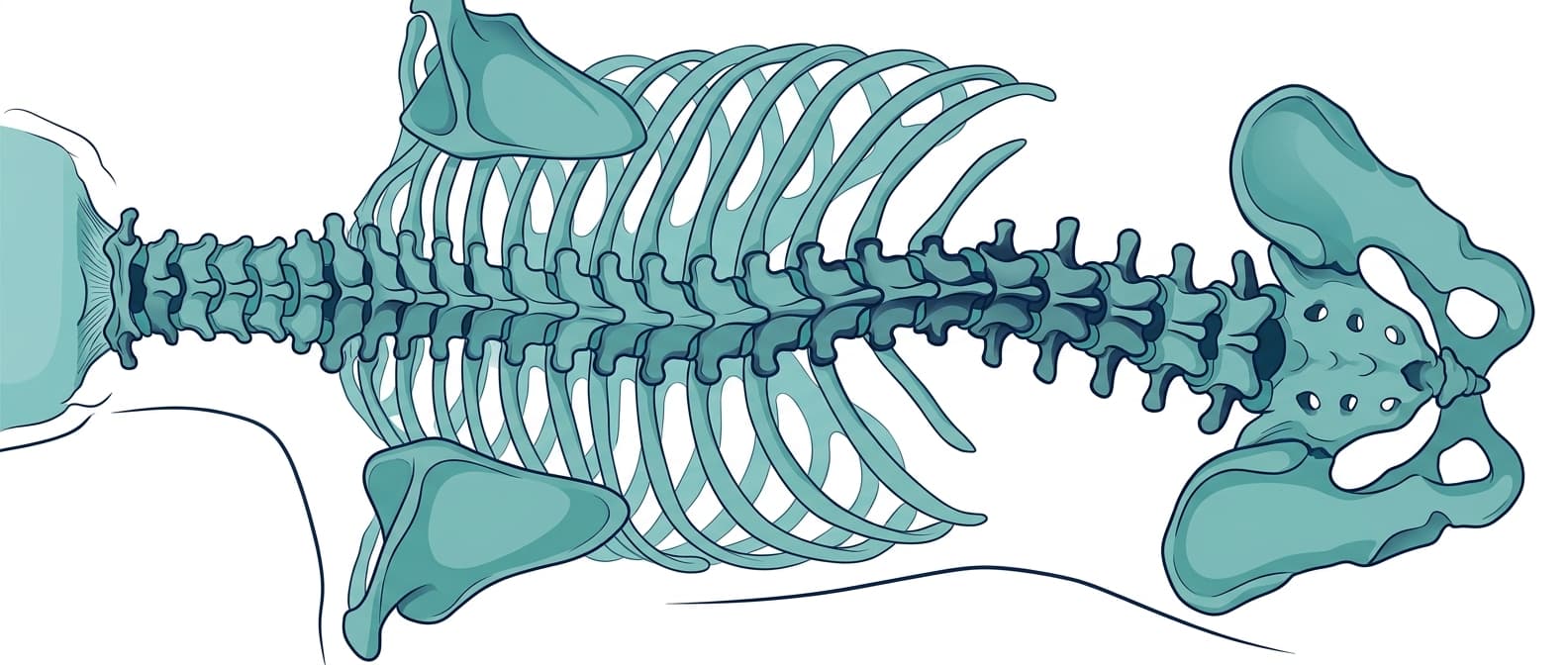
Adolescent idiopathic scoliosis, or AIS, is a condition that often catches parents off guard. It's a three-dimensional curvature of the spine that typically appears during the rapid growth spurt of puberty. While it can affect boys, AIS is significantly more common in girls, usually between the ages of 10 and 15. The "idiopathic" part simply means we don't know exactly why it happens, which can be frustrating, but it also means it's not caused by anything you or your child did wrong. Detecting scoliosis early is incredibly important because intervention, if needed, is most effective while your child is still growing.
Screening for Scoliosis
Screening for scoliosis traditionally happens in a couple of ways. Many schools still conduct basic screenings, often performed by a school nurse. Your pediatrician will also typically include a scoliosis check as part of routine physical exams, especially during the pre-teen and early teen years. These screenings usually involve the Adams forward bend test. Your child will bend forward at the waist, with their feet together and arms hanging freely, letting you or the examiner look for any asymmetry in the back, like one side of the rib cage being higher than the other, or a prominent shoulder blade.
A scoliometer is a simple, non-invasive tool often used during this screening. It's like a level that measures the angle of trunk rotation. If the scoliometer reading indicates an angle greater than 5-7 degrees, it suggests a potential curve and usually warrants a referral to an orthopedic specialist for further evaluation. It's important to understand that these screenings are exactly that: screenings. They don't diagnose scoliosis. They simply identify children who might have it and need a more definitive assessment. That assessment almost always involves an X-ray to visualize the spine and measure any curves.
Understanding Cobb Angle Measurements
When your child sees an orthopedic specialist, the primary diagnostic tool will be an X-ray of their spine. On these X-rays, the doctor measures the curve using something called the Cobb angle. This measurement is critical because it dictates the treatment pathway. The Cobb angle is calculated by drawing lines from the most tilted vertebrae at the top and bottom of the curve, then measuring the angle where those lines intersect.
Here’s what those measurements generally mean:
- 10-25 degrees: If your child has a Cobb angle in this range, it's considered mild scoliosis. The usual recommendation is careful observation. This means regular follow-up appointments, often every 4-6 months, with repeat X-rays to monitor if the curve is progressing. For many children, these mild curves don't get worse and never require bracing or surgery.
- 25-45 degrees: Curves in this range are moderate. For a growing child, particularly a girl who hasn't finished puberty, this is the threshold where bracing is typically recommended. The goal of bracing is to prevent the curve from getting worse, not to correct it entirely.
- 45+ degrees: When a curve reaches 45 degrees or more, especially if it continues to progress despite bracing, or if it's diagnosed at this severity, surgery becomes a serious consideration. At this magnitude, curves are more likely to worsen into adulthood and potentially cause issues like back pain or, in rare severe cases, affect lung function.
Remember, these are general guidelines. The decision-making process also takes into account your child's remaining growth, their age, the specific location of the curve, and how much skeletal maturity they have left (often assessed by looking at bone development on the X-ray, like the Risser sign).
Modern Bracing Options
If your child's curve falls into the moderate range (25-45 degrees) and they still have significant growth remaining, bracing will likely be recommended. The science behind bracing has evolved considerably. Bracing doesn't reverse a curve, let's be clear about that. Its primary purpose is to stop the curve from getting worse and ideally prevent the need for surgery. It's a treatment that requires immense commitment from both the child and the parents.
There are several types of braces commonly used today:
- Boston Brace (TLSO): This is perhaps the most well-known type of brace. It's a low-profile, custom-molded plastic orthosis that fits snugly around the torso, from just under the arms down to the hips. It applies pressure to specific areas of the spine to hold it in a straighter position. The Boston brace is typically worn for 18-23 hours a day. This extensive wear time can be challenging for teenagers, as it impacts daily activities and body image.
- Providence Nighttime Brace: This brace is designed to be worn only at night, usually for 8-10 hours. It works by overcorrecting the curve while the child is lying down. It's often bulkier than a Boston brace but offers the advantage of not being worn during school or social activities. The Providence brace is typically used for single curves or specific curve patterns and is a good option for kids who are highly motivated but struggle with daytime brace wear.
- Rigo Cheneau Brace: This is a more recent advancement, gaining popularity for its corrective capabilities. Unlike the Boston brace, which primarily aims to prevent progression, the Rigo Cheneau brace is designed with specific expansion areas to de-rotate and actively correct the curve in three dimensions, not just prevent it from getting worse. It's also custom-molded and often worn for 18-23 hours a day, similar to the Boston brace.
The effectiveness of bracing depends heavily on consistent wear. An orthopedic specialist and orthotist (the person who custom-fits the brace) will work closely with your family. They'll explain the specific goals for your child's brace and what to expect. Wearing a brace is a significant undertaking for a teenager, and it's normal for them to experience discomfort, frustration, and self-consciousness. Support and open communication are absolutely essential.
When Surgery Is Needed
For some children, despite observation or bracing, the curve continues to progress, reaching or exceeding 45-50 degrees. At this point, or if the curve is very severe at diagnosis, surgery becomes the most effective option to correct the curvature and prevent further progression. The decision for surgery is never taken lightly. It involves a detailed discussion with your orthopedic surgeon about the risks, benefits, and long-term implications.
The most common surgical procedure for AIS is posterior spinal fusion (PSF). During this operation, the surgeon accesses the spine from the back. They use a combination of metal rods, screws, and hooks to carefully straighten the curved section of the spine. Small pieces of bone graft (either from the patient, a donor, or synthetic material) are then placed around the instrumentation. Over several months, these bone grafts fuse the vertebrae together, creating a solid, stable segment of the spine. This fusion prevents further curvature in the instrumented section. PSF is a highly effective procedure, with excellent long-term outcomes for correcting severe curves.
A newer and less common surgical option, primarily for select patients who are still growing, is vertebral body tethering (VBT). Instead of fusing the spine, VBT uses a flexible cord (the "tether") anchored by screws to the front of the vertebral bodies along the convex side of the curve. The idea is that as your child grows, the tether restricts growth on the convex side, allowing the concave side to catch up, thereby correcting the curve. This is sometimes called "growth modulation." VBT is less invasive than PSF, often performed through small incisions, and maintains more spinal flexibility. However, it's not suitable for all curve types or all patients. It requires a specific amount of remaining growth, and the long-term results are still being studied compared to the decades of data we have for PSF. There's also a risk of overcorrection or undercorrection, and sometimes the tether can break. Your surgeon will discuss if VBT is a viable option for your child, weighing its potential benefits against its specific considerations.
Recovery Realities
No matter which surgical path is chosen, recovery is a significant process. For posterior spinal fusion, your child will typically spend 3-7 days in the hospital. Pain management is a major focus immediately after surgery, often involving intravenous pain medication and then transitioning to oral medication. The first few days involve getting out of bed and walking with assistance. Most children can return to school within 2-4 weeks, though they might need a lighter schedule initially. Strenuous activities, heavy lifting, and contact sports are usually restricted for 6-12 months to allow the fusion to solidify completely. Full recovery, where the bone is completely fused, takes about a year.
Vertebral body tethering generally involves a shorter hospital stay, often 2-4 days, and a somewhat quicker initial recovery. Because there's no fusion, the restrictions on activity might be less stringent, and return to sports can sometimes be sooner, perhaps within 3-6 months. However, it's still major surgery, and your child will experience pain and fatigue. The recovery, while potentially faster, still requires patience and adherence to the surgeon's instructions to allow the body to heal and the tether to do its work.
As a parent, you'll need to be prepared for the emotional and physical demands of recovery. Your child will need your support and encouragement. It's a marathon, not a sprint, but the vast majority of children who undergo scoliosis surgery go on to live very active and healthy lives.
Long-Term Life with Scoliosis
Life with scoliosis, whether treated with observation, bracing, or surgery, generally has excellent long-term outcomes. For those who manage their curves with observation or bracing, most lead normal lives with minimal issues. Some adults who were braced might experience mild, non-disabling back pain, but this is often no different than the general population. Regular exercise and maintaining core strength are always beneficial.
For individuals who undergo spinal fusion surgery, satisfaction rates are very high. The corrected curve is stable, and the vast majority of patients live active, fulfilling lives. They can participate in most sports and activities, though some contact sports might carry a slightly higher risk of injury to the unfused segments above or below the fusion. There can be a slight loss of spinal flexibility in the fused segment, but the spine is designed to move, and the unfused segments compensate well. Over time, some patients might experience mild back pain, similar to the general population, or occasionally need follow-up for hardware removal if it causes irritation.
With VBT, since it's a newer procedure, the very long-term outcomes are still being collected. The hope is for continued flexibility and growth, leading to a more natural-looking spine. However, as mentioned, there's a possibility of the curve progressing again, or requiring a secondary procedure if the tether breaks or causes problems.
Regardless of the treatment path, living with scoliosis means living with a unique spinal anatomy. Regular check-ups with your orthopedic specialist, maintaining a healthy lifestyle, and listening to your body are always good practices.
Talking to Your Teenager About Bracing
This is perhaps one of the most challenging aspects of managing scoliosis. Asking a teenager, especially a girl, to wear a brace for 18-23 hours a day is a monumental request. Their self-image, social life, and sense of normalcy are paramount at this age.
Here's how to approach it:
- Be Empathetic and Listen: Acknowledge their feelings. It's okay for them to be angry, sad, or frustrated. Don't dismiss their concerns. Ask them what worries them most.
- Educate Together: Involve them in the process. Have them meet the orthotist who will make their brace. Let them choose colors or patterns if available. Understanding why they need the brace and what it does can help them accept it.
- Focus on the Future: Remind them that the brace is a temporary tool for a long-term benefit. It's an investment in their spinal health, potentially preventing a more drastic intervention like surgery later.
- Find Role Models/Support: Connect with other teens who have worn braces. Online communities or local support groups can provide a sense of not being alone. Seeing others thrive while wearing a brace can be incredibly motivating.
- Integrate It into Life: Help them find clothing that conceals the brace comfortably. Encourage them to continue their normal activities as much as possible. The goal isn't to hide it, but to make it part of their routine without it defining them.
- Praise Effort, Not Just Compliance: Acknowledge how hard they are working. Even a few hours of brace wear is an effort. Celebrate small victories.
- Compromise and Flexibility: While consistent wear is key, there might be specific events (like a school dance or a special occasion) where a few hours out of the brace might be negotiated, with the understanding that they'll make up for it. Open communication with your doctor about this is always best.
This isn't about forcing compliance; it's about building a partnership with your teenager to navigate a difficult situation together. Their emotional well-being is just as important as their physical health.
If you notice any signs of scoliosis in your child, such as uneven shoulders, one hip appearing higher than the other, or a prominent rib cage when they bend forward, it's time to talk to their pediatrician. If a scoliometer reading indicates a potential curve, or if your child's pediatrician recommends it, seeking an evaluation from an orthopedic surgeon specializing in pediatric spinal conditions is the next crucial step. Early detection and expert guidance are your best allies in managing adolescent idiopathic scoliosis.