That first step out of bed in the morning — the one that makes you wince and limp to the bathroom — is one of the most recognizable symptoms in all of orthopaedics. If you've experienced it, you probably already know the diagnosis: plantar fasciitis.
It's the most common cause of heel pain, affecting roughly 2 million Americans every year. And yet most people who have it either wait too long to address it or attack it with the wrong treatments. Here's what actually works and what you can skip.
What's happening in your heel
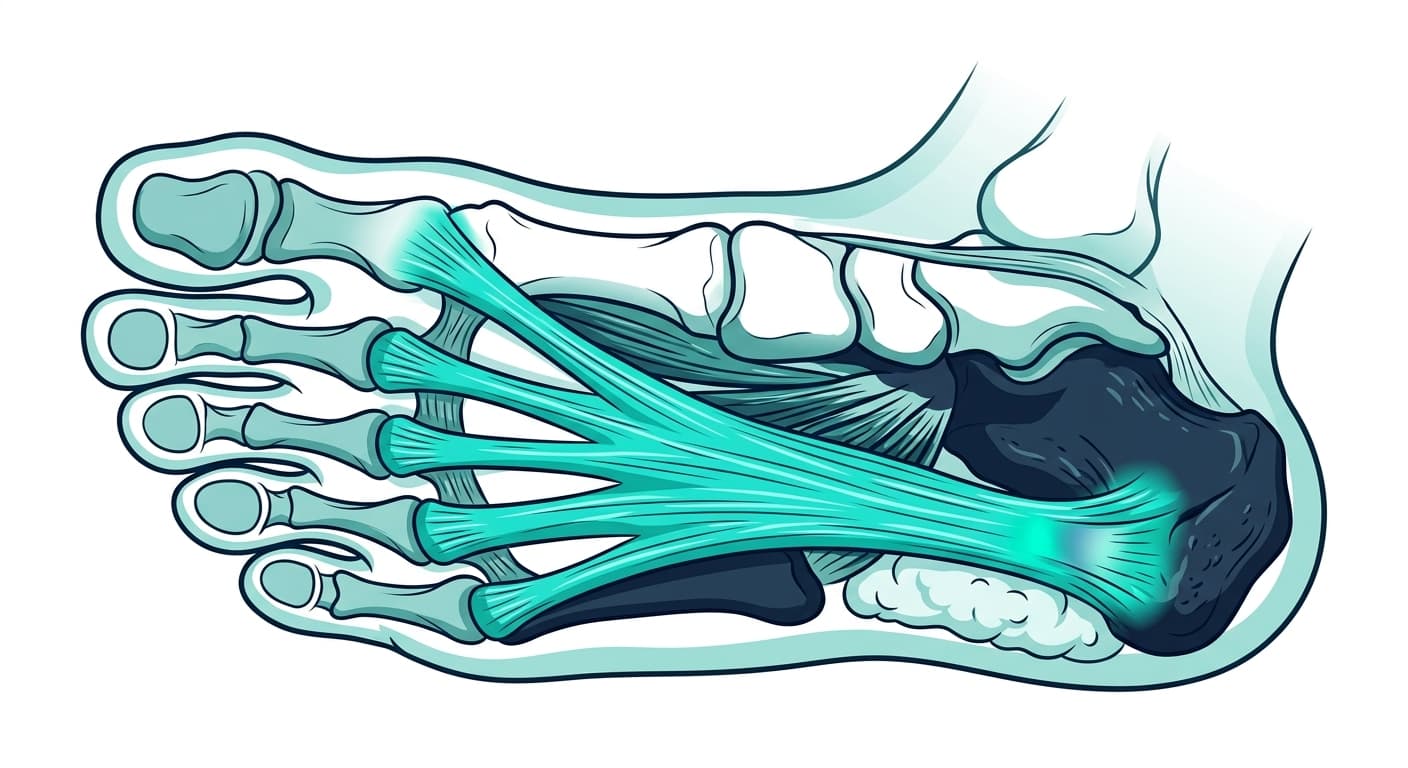
The plantar fascia is a thick band of tissue running along the bottom of your foot, connecting your heel bone to your toes. It acts as a shock absorber and supports the arch when you walk, run, or stand.
Plantar fasciitis isn't really an inflammatory condition — despite the "-itis" suffix suggesting inflammation. Research over the past two decades has shown that what's happening is more accurately described as degeneration of the fascia tissue itself, particularly where it attaches to the heel. Repetitive stress causes tiny tears that don't fully heal, and the tissue gradually breaks down.
The classic morning pain happens because the fascia tightens overnight while you sleep. When you take that first step, you're suddenly stretching a structure that's been contracted for hours. As you walk around and it loosens up, the pain usually improves — only to creep back after long periods of sitting or standing.
Who gets it
Anyone can develop plantar fasciitis, but it's most common in people who:
- Are between 40 and 60 years old
- Spend long hours on their feet (teachers, nurses, restaurant workers, retail employees)
- Have recently increased their running mileage or started a new exercise program
- Are overweight — every extra pound adds significant load to the plantar fascia
- Have either flat feet or high arches, both of which alter how load is distributed
- Wear shoes with poor arch support or walk barefoot on hard floors regularly
Runners get it frequently, but it's just as common in sedentary adults who simply stand a lot. It doesn't discriminate.
Making the diagnosis
Plantar fasciitis is almost always a clinical diagnosis — meaning your doctor can identify it by listening to your symptoms and examining your foot. There's a characteristic pattern: pain at the bottom of the heel, worst in the morning or after rest, that improves with movement but returns after prolonged activity.
Pressing directly on the medial calcaneal tubercle (the spot on the inside of your heel where the fascia attaches) usually reproduces the pain exactly.
Imaging is rarely needed initially. X-rays are often done but don't show soft tissue — what they do reveal is a heel spur, a bony protrusion at the fascia attachment site. Heel spurs get blamed for plantar fasciitis constantly, but this is mostly wrong. Heel spurs are present in people without any heel pain, and they're absent in plenty of plantar fasciitis cases. The fascia degeneration is the problem, not the spur.
MRI is reserved for cases where the diagnosis is unclear or symptoms aren't responding to treatment as expected.
What to try first
The good news: the vast majority of plantar fasciitis cases resolve without surgery. Studies put the success rate of conservative treatment somewhere between 80 and 90 percent over 12 months. The less good news: it takes patience, and some approaches require consistent daily effort that many people give up on before they work.
Stretching is the cornerstone. Two stretches in particular have the strongest evidence:
The plantar fascia stretch: Sit down, cross your affected foot over your knee, and pull your toes back toward your shin until you feel a stretch along the bottom of your foot. Hold for 10 seconds, repeat 10 times. Do this before you take your first step in the morning — literally before your foot touches the floor.
The calf/Achilles stretch: Tight calf muscles increase tension on the plantar fascia. Stand facing a wall, step your affected foot back, keep the heel flat on the floor, and lean forward until you feel the stretch. Both with a straight knee and a bent knee — these target different parts of the calf complex.
Do both multiple times daily. Not once. Multiple times. Patients who see results from stretching are almost always the ones who actually did it every time they sat down.
Supportive footwear all day, every day. This is harder than it sounds. Good arch support means while you're walking around your house, too — not just shoes you put on to leave. Going barefoot on hard floors is one of the most reliable ways to slow recovery. Bring your shoes to the bathroom in the morning before your foot hits the tile.
Over-the-counter insoles add cushioning and arch support. Custom orthotics aren't necessary for most people — a $30 pair of Superfeet or similar arch supports works for the majority of cases. Custom orthotics have a place, but they're often prescribed prematurely.
NSAIDs (ibuprofen, naproxen) can manage pain and may reduce local irritation, particularly during flare-ups. They're not a fix on their own.
Ice after activity helps. Roll a frozen water bottle under your foot for 10–15 minutes after a long day on your feet.
Activity modification doesn't mean stopping everything. It means temporarily reducing high-impact activity (running, jumping, long walks on hard pavement) while keeping up low-impact movement like swimming or cycling.
When first-line treatment isn't enough
If stretching, footwear changes, and NSAIDs haven't produced meaningful improvement after six to eight weeks, a few additional options are worth discussing with an orthopaedic specialist or podiatrist:
Night splints hold your foot in slight dorsiflexion while you sleep, keeping the plantar fascia at length overnight. They prevent that morning tightening that causes the signature first-step pain. They're uncomfortable to sleep in, and compliance is the main challenge — but for patients who use them consistently, results are often faster than stretching alone.
Physical therapy adds value, particularly for patients who need manual therapy to loosen the calf and Achilles, guidance on correcting gait mechanics, or a structured progression of strengthening exercises. There's growing evidence for eccentric heel drop exercises specifically.
Corticosteroid injections provide short-term pain relief — often significant relief — in many patients. The trade-off: repeated injections increase the risk of plantar fascia rupture and fat pad atrophy, which can create new problems. Most specialists limit to one or two injections before reconsidering this approach.
Platelet-rich plasma (PRP) injections have gained traction in recent years. The evidence is mixed — some studies show benefit over cortisone in terms of longer-lasting relief and lower rupture risk, others show no clear advantage. It's not typically covered by insurance. It may be a reasonable consideration for patients who've failed cortisone and want to avoid surgery.
Extracorporeal shockwave therapy (ESWT) delivers acoustic pulses to the heel to stimulate healing. Evidence supports its use for chronic plantar fasciitis (symptoms lasting more than six months) that hasn't responded to other measures. Multiple sessions are required and insurance coverage varies.
Surgery: the last resort
Surgery for plantar fasciitis is uncommon. Less than 5 percent of patients eventually need it, and most specialists won't discuss it until at least 12 months of consistent conservative treatment has failed.
The standard procedure is a plantar fasciotomy — partially releasing the fascia to reduce tension at the heel attachment. It can be done open or endoscopically through small incisions. Results are generally good for well-selected patients, with 70–90 percent reporting significant improvement.
The downside of releasing the plantar fascia is that it changes the biomechanics of the foot. A small percentage of patients develop arch collapse or lateral column pain afterward. It's effective, but it's not a minor procedure in terms of its structural implications.
Heel spur removal is sometimes done at the same time but is generally considered unnecessary unless the spur is itself causing mechanical problems — which is rare.
How long does it actually take
This is the question everyone asks and nobody likes the answer to. Most people with plantar fasciitis who follow through on conservative treatment see meaningful improvement within three to six months. Complete resolution — where it genuinely stops bothering you — sometimes takes a year.
The cases that drag on longest are usually the ones where people did stretching inconsistently, kept walking barefoot at home, wore unsupportive shoes, or expected one cortisone shot to solve everything.
The cases that resolve fastest are the ones where people committed to stretching multiple times daily, wore shoes from the moment they woke up, reduced high-impact activity, and stayed patient.
Neither outcome is random. What you do every day matters significantly more than any single treatment.
When to see a specialist
See an orthopaedic surgeon or sports medicine physician if:
- Your pain hasn't improved after six to eight weeks of consistent stretching and footwear changes
- The pain is severe enough to affect how you walk or do your job
- You're not sure whether the diagnosis is correct — there are other causes of heel pain (nerve entrapment, stress fracture, Achilles tendinopathy) that need different treatment
- You've had one or more cortisone injections without lasting benefit
Most cases don't require surgery — but getting the right diagnosis and a structured plan earlier tends to produce faster results than managing it alone for a year before seeking help.