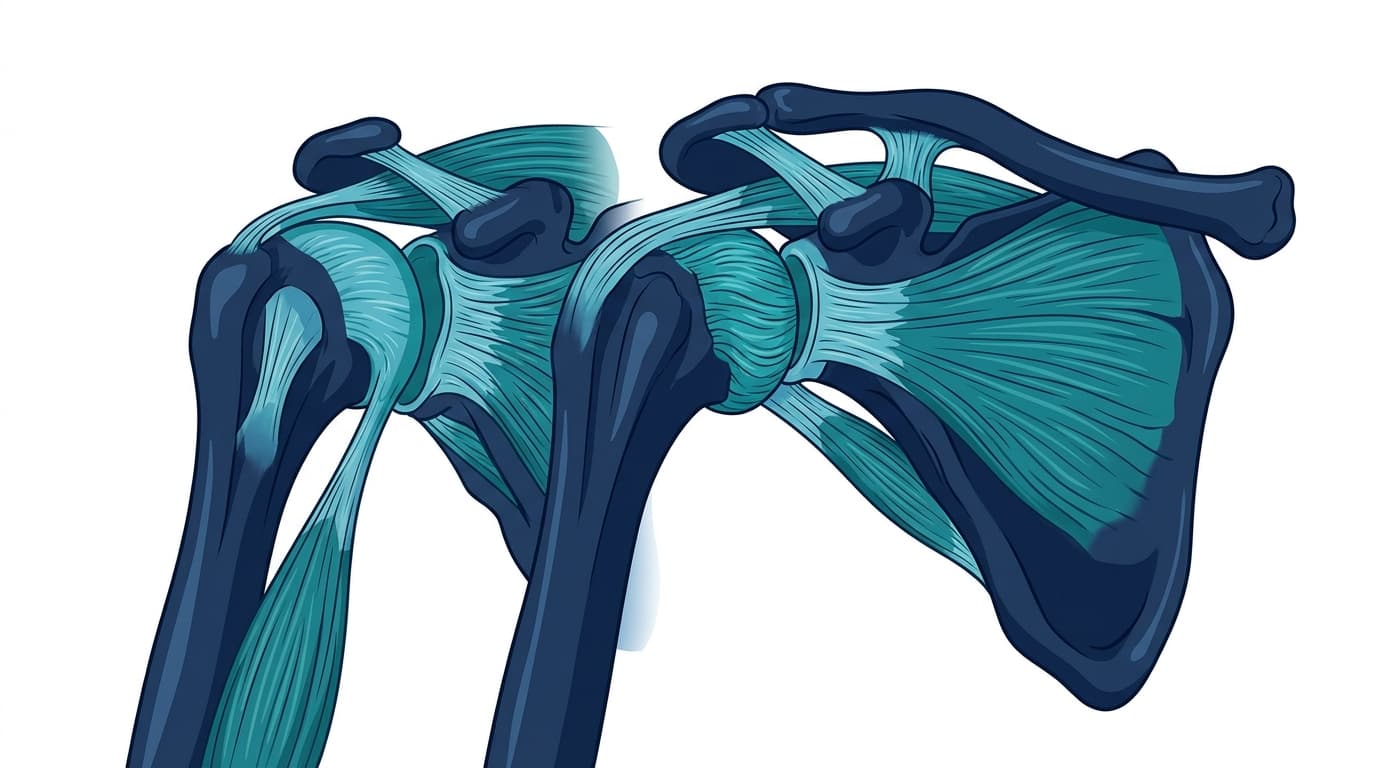
Frozen shoulder is one of the most maddening orthopaedic conditions to live with. Your shoulder slowly stiffens over months until you can't reach behind your back, can't sleep on that side, can't take off your jacket. Then, eventually, it loosens up and goes away on its own. The whole arc takes 18 to 30 months. During the worst of it, the joint really does feel broken.
The medical name is adhesive capsulitis. The capsule that surrounds the shoulder joint thickens and tightens until the head of your humerus can barely move inside it. We don't know exactly why this starts. It happens more in women than men, more after age 40, and a lot more in people with diabetes. Sometimes it follows a minor shoulder injury, surgery, or an extended period of disuse. Often it appears for no reason anyone can identify.
The good news is that most patients eventually recover, with or without treatment. The bad news is that the timeline is long enough that most people aren't willing to wait it out. Here's how the treatment ladder actually works in practice, from the gentlest first step to the most aggressive surgical option.
Start with PT and a careful injection
For most patients, this is where the journey begins and where it ends. Physical therapy, focused on stretching and range-of-motion work, gradually convinces the capsule to release. Stretches are uncomfortable but should not be agonizing. Pushing through severe pain inflames the joint and slows everything down. Working at the edge of discomfort, multiple times a day, is the pace that produces results.
Heat helps. Fifteen minutes with a heating pad before stretching makes the tissue more pliable, in the same way you'd warm up a tight hamstring before a run. NSAIDs like ibuprofen or naproxen take the edge off the inflammation that builds up after PT sessions. They aren't a treatment, they're a tolerance aid.
A single corticosteroid injection during the painful "freezing" phase often pays for itself. The shot quiets the inflammation enough that PT becomes possible instead of dreaded. Most specialists won't repeat injections more than once or twice. Repeated steroids in the same joint cause cartilage problems and don't add much benefit beyond the first one.
For patients who commit to home stretching every single day for three to four months, this combination resolves the majority of cases. The patients who fail conservative treatment usually fall into one of two camps: they didn't actually do the stretches consistently, or they have diabetes.
Hydrodilatation: the next escalation
When PT plus injection isn't moving the needle after a few months, hydrodilatation is worth a conversation. The procedure is simple in concept. Under ultrasound guidance, a needle goes into the shoulder joint, and the radiologist or sports medicine doc injects 20 to 40 milliliters of fluid (saline plus steroid plus a local anesthetic) under enough pressure to mechanically stretch the capsule from the inside.
You feel it. There's a real sensation of pressure as the capsule expands. Some patients describe a popping sensation as small adhesions break apart.
Studies consistently show 60 to 70 percent of patients in the early frozen phase get meaningful improvement from a single session. The catch is that hydrodilatation only works if you go straight into aggressive PT afterward. The capsule will tighten back up within days if you don't. Patients who get the injection and then don't show up to therapy waste the procedure.
Manipulation under anesthesia
For the patient who has plateaued in the frozen phase, hasn't responded to less invasive options, and is months into a stalled recovery, MUA enters the conversation. The surgeon takes the patient under general anesthesia, then forcefully moves the shoulder through its full range of motion. With the muscles fully relaxed, the surgeon can mechanically tear the adhesions that keep the joint stuck. There's often an audible pop as the capsule releases.
Done well, by an experienced shoulder surgeon, MUA can restore most of a patient's range of motion in a single procedure. The recovery is identical to hydrodilatation: PT starts that same afternoon or the next morning, and stays aggressive for weeks. Wait three days and the capsule re-scars.
The risk that gets discussed most is humerus fracture, which is real but rare with experienced hands. Less commonly, the procedure can cause nerve injury or shoulder dislocation. MUA isn't right for every patient. It works best on a true frozen-phase shoulder where the capsule is tight but not yet thickly scarred. In intensely painful freezing-phase shoulders, the inflammation makes manipulation risky and less effective.
Arthroscopic capsular release
Surgery is the right call for two groups: patients who failed 6 to 12 months of conservative treatment and want their lives back, and severe diabetics whose frozen shoulders rarely resolve without surgical help. The procedure is minimally invasive. Two or three incisions, each smaller than a centimeter, give the surgeon access to the joint with a camera and small cutting instruments. The thickened, tight portions of the capsule are cut and released. Inflamed tissue is cleaned out at the same time.
What follows is the part nobody loves. PT starts on day one, sometimes within hours of the surgery. Patients are often sent home with a continuous passive motion machine that slowly cycles the arm through its range while they watch TV or sleep. Maintaining the gained motion for the first two weeks is everything. Without aggressive early movement, the capsule scars right back down and the surgery is wasted.
Full functional motion typically returns in three to six months. The relief, for patients who've been stuck for a year or more, is real. Most are extraordinarily glad they did it after the fact, even though the recovery is grinding.
Why diabetics get this so much worse
Frozen shoulder behaves differently in diabetics, and it's worth understanding why. Elevated blood sugar levels over time cause something called advanced glycation. Sugar molecules cross-link to proteins throughout the body's connective tissue, making collagen stiffer and less elastic. The shoulder capsule in a diabetic patient is genuinely thicker and tougher than the same capsule in a non-diabetic. It resists stretching. It scars more readily after manipulation.
For type 1 diabetics in particular, frozen shoulder rates run two to four times higher than the general population, and the cases tend to be more severe and last longer. Conservative treatment fails more often. Surgical release is needed sooner. None of this is the patient's fault, but it does shift the calculation about when to escalate.
How to think about timing
The honest version of frozen shoulder counseling looks something like this. If you're in month two or three and PT plus an injection seems to be helping at all, give it more time. The freezing-to-thawing transition can take a year. Most patients who eventually recover do so without surgery.
If you're at six months with no measurable progress, your shoulder is severely limiting daily life, and your symptoms haven't shifted from one month to the next, the conversation about hydrodilatation, MUA, or arthroscopic release becomes reasonable. There's no medal for waiting it out, and a surgical or procedural intervention can compress 18 months of suffering into 4 months of structured recovery.
If you have diabetes, particularly poorly controlled diabetes, the threshold for escalating is lower. Don't sit in conservative care for a year hoping for improvement that statistically isn't coming.
See an orthopaedic shoulder specialist if your shoulder pain and stiffness has worsened over more than four to six weeks, your range of motion is dropping rather than holding steady, or basic rest and over-the-counter medication isn't taking the edge off. They can confirm the diagnosis (rotator cuff pathology and arthritis can mimic adhesive capsulitis), stage where you are in the freezing-frozen-thawing arc, and lay out a treatment plan that fits your timeline and your tolerance for invasiveness. The earlier the right diagnosis happens, the more options you have.