Hallux Rigidus
Hallux rigidus is arthritis of the big toe joint—specifically the metatarsophalangeal (MTP) joint at the base of the great toe. It is the most common arthritic condition of the foot, affecting roughly 1 in 40 adults over 50. The cartilage covering the joint surfaces wears away, bone spurs (osteophytes) develop around the joint, and motion becomes progressively restricted and painful. "Hallux rigidus" means literally stiff big toe—and the progressive loss of dorsiflexion (the ability to bend the toe upward) is what drives most of the functional limitations.
Find a Specialist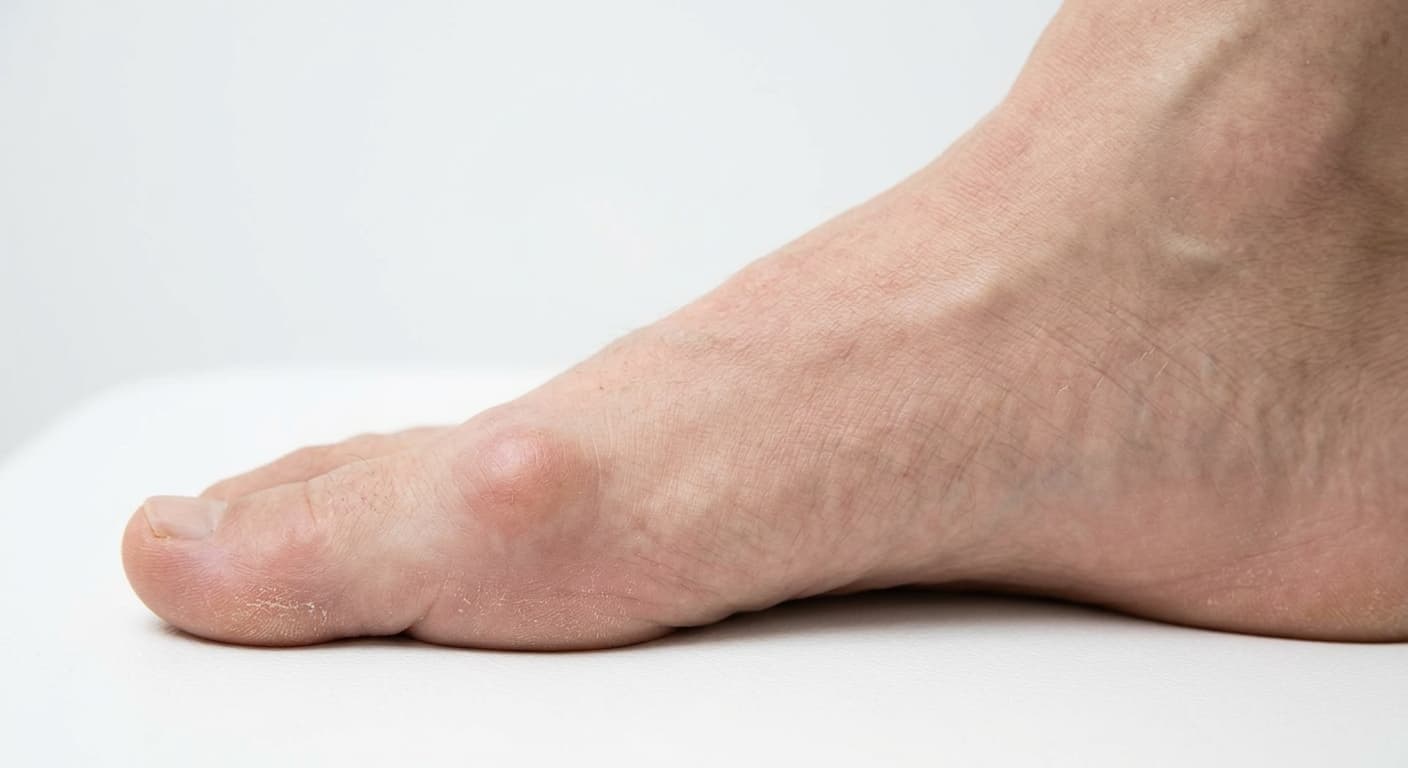
Symptoms
- Pain and stiffness at the base of the big toe, especially with pushing off while walking
- Difficulty bending the big toe upward (reduced dorsiflexion)
- A visible bony bump on top of the joint
- Pain that worsens in cold or damp weather
- Swelling and inflammation around the joint after activity
- A tendency to walk on the outer edge of the foot to avoid loading the toe
When to See a Doctor
See a foot and ankle specialist if big toe pain is limiting your walking, exercise, or footwear choices. Hallux rigidus is progressive—treatment is more straightforward in earlier stages before significant bone spur formation and cartilage loss.
Treatment Options
Shoe modifications and orthotics
Stiff-soled shoes, rocker-bottom soles, and custom orthotics reduce the bending demand on the toe joint. Carbon fiber insoles are commonly used. This is often the first-line approach.
Corticosteroid injection
Provides temporary pain relief and reduces inflammation, useful for acute flares. Effect typically lasts weeks to a few months.
Cheilectomy
Surgical removal of the bone spurs around the joint while preserving the joint. Effective in mild to moderate hallux rigidus, particularly when the main problem is dorsal impingement (hitting the top bone spurs). Most patients see significant pain relief and some improvement in motion.
Fusion (arthrodesis)
The joint surfaces are removed and the bones are fused in a fixed position. The gold standard for severe hallux rigidus. Eliminates pain reliably; the trade-off is permanent loss of toe joint motion, which affects shoe choice (heeled shoes become difficult).
Joint replacement (implant arthroplasty)
An alternative to fusion that preserves some motion, though longer-term outcomes are less well-established than fusion. Better suited to lower-demand patients.
Recovery Timeline
Cheilectomy: weight-bearing in a surgical shoe within days, return to regular shoes in 4–6 weeks, full activity by 3 months. Fusion: non-weight-bearing for 6–8 weeks, walking in regular shoes by 10–12 weeks, full recovery in 4–6 months. Bone healing is monitored with X-rays.
Frequently Asked Questions
Is hallux rigidus the same as a bunion?
No. A bunion (hallux valgus) is a deformity in which the big toe drifts toward the second toe, creating a bump on the inner side of the foot. Hallux rigidus is arthritis of the same joint, creating a bump on top of the foot from bone spurs. Both can be painful; both are treated by foot and ankle specialists; and they can coexist, but they are different conditions requiring different surgical approaches.
Can I still run or play sports with hallux rigidus?
Many people continue to exercise with early hallux rigidus using stiff-soled shoes and activity modifications. High-impact running and sports that require toe-off (sprinting, jumping) become progressively harder as the condition advances. After fusion surgery, running and most sports remain possible, though cleated shoes can be difficult.
What type of doctor treats hallux rigidus?
Foot and ankle orthopaedic surgeons and podiatrists both treat hallux rigidus. For surgical cases—particularly fusion—look for a surgeon who has specific foot and ankle fellowship training.
Related Specialty
Foot & Ankle Specialists →Related Procedures
Hallux Rigidus by State
Related Conditions
This information is for educational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.