Knee Bursitis
Bursae are small fluid-filled sacs that cushion bones, tendons, and muscles around joints. The knee has around 11 bursae, and several are prone to irritation and swelling. Prepatellar bursitis (swelling directly over the kneecap) is the most common type, often from prolonged kneeling—which is why it is sometimes called "housemaid's knee" or "plumber's knee." Pes anserine bursitis affects the inner side of the knee just below the joint and is common in older adults with osteoarthritis.
Find a Specialist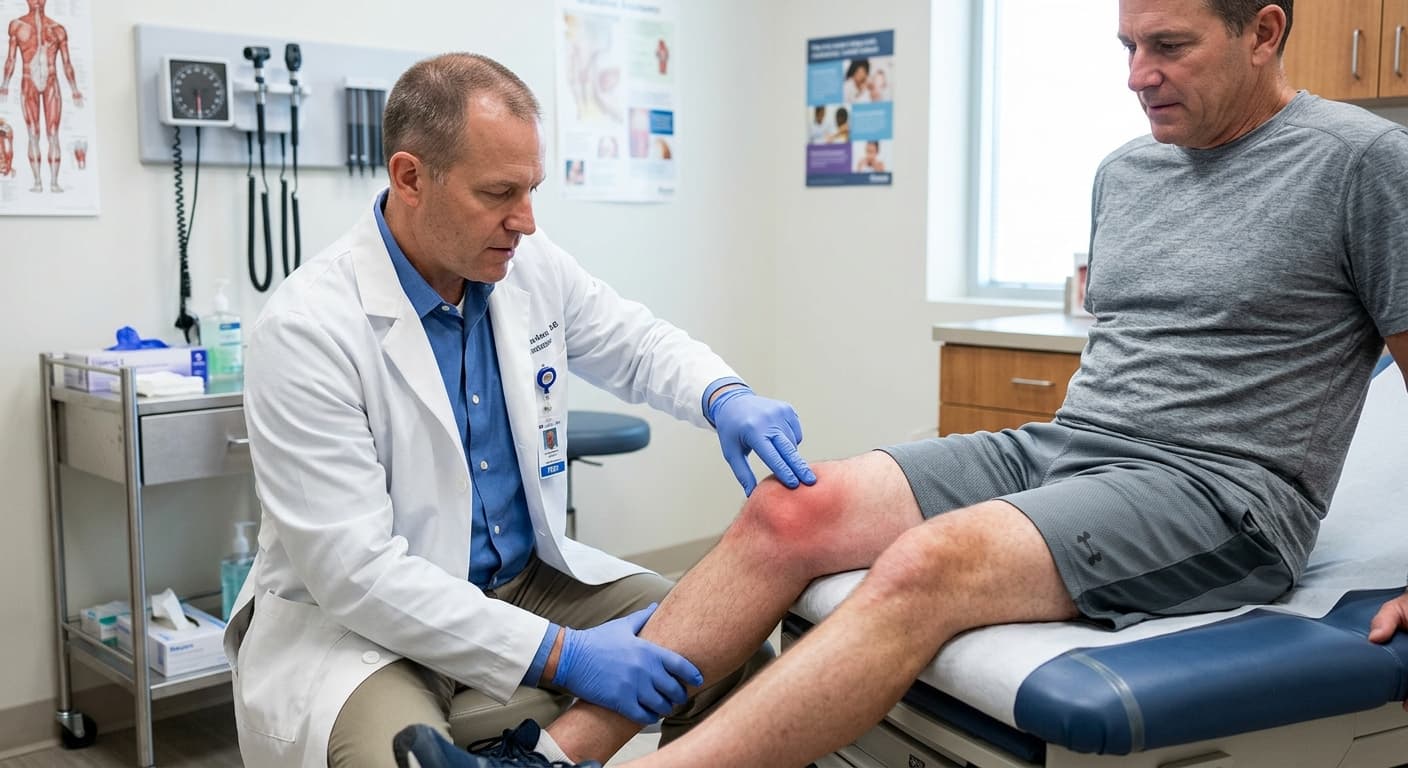
Symptoms
- Visible swelling directly over or around the kneecap
- Tenderness when pressing on the swollen area
- Warmth and redness over the affected bursa
- Pain that worsens with kneeling or direct pressure on the knee
- Stiffness, particularly after rest
- Fever and increased redness (if the bursa is infected—septic bursitis)
When to See a Doctor
See a doctor if knee swelling is warm, red, and accompanied by fever—infected bursitis needs prompt antibiotic treatment or drainage. Non-infectious bursitis that does not improve with rest and ice after a week or two also warrants evaluation.
Treatment Options
Rest and ice
Avoiding kneeling and direct pressure on the affected bursa is often enough to resolve mild bursitis over 1–3 weeks. Ice for 15–20 minutes several times daily reduces swelling.
Aspiration
A needle is used to drain the fluid from the swollen bursa in the office. Provides immediate relief. The fluid is sent for lab analysis to rule out infection or gout crystals.
Corticosteroid injection
After aspiration or on its own, a cortisone injection into the bursa reduces inflammation and lowers the chance of fluid reaccumulating. Effective for most non-infectious cases.
Antibiotic treatment
Infected (septic) bursitis requires antibiotics, usually oral but sometimes IV depending on severity. Drainage of the infected bursa may also be needed.
Surgical bursectomy
Removal of the bursa is rarely needed but considered for chronically recurrent bursitis that does not respond to other treatments.
Recovery Timeline
Most non-infectious bursitis resolves within a few weeks with conservative care. Aspiration and injection usually resolve symptoms within days to weeks. Septic bursitis clears with antibiotics in 1–3 weeks but needs close follow-up. Recurrence is common if the underlying activity or pressure on the knee continues.
Frequently Asked Questions
How do I tell knee bursitis from a meniscus tear?
The location and feel of the swelling are different. Bursitis swelling is soft, visible, and sits on the surface directly over or below the kneecap—you can feel a distinct fluid-filled lump. Meniscus tear swelling is inside the joint, causing generalized joint-line swelling with locking or clicking. An orthopaedic exam usually distinguishes the two, with MRI used to confirm a meniscus tear.
Can knee bursitis come back?
Yes, especially if you return to activities that involve repeated kneeling or pressure on the knee. Knee pads, technique modification, and addressing contributing factors like obesity or osteoarthritis lower the risk of recurrence. Some patients with chronic, recurrent bursitis eventually opt for bursectomy to permanently remove the problematic bursa.
What type of doctor treats knee bursitis?
Primary care physicians, sports medicine doctors, and orthopaedic surgeons all treat knee bursitis. Sports medicine doctors or orthopaedic surgeons are the right choice if the diagnosis is unclear, if aspiration is needed, or if the bursitis keeps coming back.
Related Specialty
Sports Med Specialists →Related Procedures
Knee Bursitis by State
Related Conditions
This information is for educational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.